Scholar Achievements
Former Scholar Dr. Jose Alejandro Rauh-Hain Receives National Institutes of Health R01 Award
 Former AAOGF Scholar, Dr. Jose Alejandro Rauh-Hain has been awarded a National Institutes of Health R01 Award to support his project Health equity in fertility specialty care among Cancer survivors
Former AAOGF Scholar, Dr. Jose Alejandro Rauh-Hain has been awarded a National Institutes of Health R01 Award to support his project Health equity in fertility specialty care among Cancer survivors
Summary: Fertility is extremely important to many young women diagnosed with cancer. The deleterious effects of cancer treatments on fertility among medically underserved cancer survivors has emerged as an important area of widening disparity in health care. The overall objective of our study is to answer two distinct questions: 1. What are the sources and extent of disparities in fertility preservation, access to ARTs, and live births among cancer survivors? 2. Does improving access to ARTs mitigate these disparities? We will evaluate how dimensions of social disparities arising from individual level, neighborhood-level (social determinants measured at census tract), and policy-level (state insurance mandates) factors affect access to and use of ARTs and live births. Specifically, we aim to 1) investigate individual-, neighborhood-, and policy-level factors associated with fertility preservation; 2) investigate individual-, neighborhood-, and policy-level factors associated with ART use after completion of cancer treatment; and 3) quantify the contribution of individual-, neighborhood-, policy-level factors to live birth rates after cancer, and whether live birth rates after cancer will be lower in medically underserved populations and partially mediated by ART use. Creation of a family is a basic human right, and ensuring equitable access to oncofertility services for all populations is key to addressing cancer care disparities for reproductive-age cancer survivors. The deleterious effects of cancer treatments on fertility among medically underserved cancer survivors has emerged as an important area of widening disparity in health care. Study findings should reveal the mechanisms underlying disparities in access to ARTs and could be used by policymakers to improve access to ARTs for vulnerable populations.
Angeles Alvarez Secord Installed as SGO President, Honored with Prestigious Award, at Annual Meeting on Women’s Cancer
 It is my privilege and honor to serve as the 55th president of the Society of Gynecology (SGO). In the spirit of unity, Dr. Ginger Gardner, the Chair of the Foundation for Women’s Cancer (FWC), and I will jointly commence the 55th year of SGO and celebrate the FWC. The theme for our year, is the “The Power of Shared Purpose: Transforming Gynecologic Cancer Care” to create a unifying culture that will maximally leverage opportunities for synergistic collaboration to further our collective mission and vision where everyone has the power to impact, prevent, overcome, and eradicate gynecologic cancers.
It is my privilege and honor to serve as the 55th president of the Society of Gynecology (SGO). In the spirit of unity, Dr. Ginger Gardner, the Chair of the Foundation for Women’s Cancer (FWC), and I will jointly commence the 55th year of SGO and celebrate the FWC. The theme for our year, is the “The Power of Shared Purpose: Transforming Gynecologic Cancer Care” to create a unifying culture that will maximally leverage opportunities for synergistic collaboration to further our collective mission and vision where everyone has the power to impact, prevent, overcome, and eradicate gynecologic cancers.
As I reflect on my career, I recognize the important role that the American Association of Obstetricians and Gynecologists Foundation (AAOGF), American Gynecological Obstetrical Society (AGOS), and the American Board of Obstetrics and Gynecology (ABOG) played in my successful journey. The career development award I received from the American Association of Obstetricians and Gynecologists Foundation (AAOGF)/American Board of Obstetrics and Gynecology (ABOG) in 2001 was instrumental in paving the pathway for my career as a physician-scientist, clinical trialist, and leader. I am thankful to AAOGF, ABOG, AGOS, and my mentors for believing in me and providing the needed tools to thrive. AAOGF in collaboration with several partners (ABOG, GOG Foundation, Burroughs Wellcome, Reproductive Scientist Development Program, Clovis Oncology, and Society for Maternal-Fetal Medicine) have been granting career development awards since 1984 with over 80 scholars in the program. In addition AAOGF, ABOG, and the American College of Obstetricians and Gynecologists support researchers through our Bridge Award program.
The SGO/FWC theme for this upcoming year was, in part, inspired by AAOGF. AAOGF has provided a stellar example of mission-driven synergistic collaboration to advance knowledge and care of our patients through the development of physician-scientists and innovative research in obstetrics and gynecology. By working with other organizations AAOGF has been able to support the development of future research leaders in obstetrics and gynecology and accelerate research that will enhance care for all our patients.
I am so thankful to be part of the AAOGF family.
Angeles Alvarez Secord
Rimel Appointed Medical Director for Cancer Clinical Trials Office at Cedars-Sinai Medical Center
BJ Rimel, MD, associate professor of Obstetrics and Gynecology at Cedars-Sinai Cancer at the Cedars-Sinai Medical Center, has been appointed as the Medical Director for the Cancer Clinical Trials Office (CCTO).
Dr. Rimel received her medical degree from Duke University School of Medicine and her residency was at Northwestern University in Obstetrics and Gynecology. She obtained a Fellowship in Gynecologic Oncology at Washington University in St. Louis.
Dr. Rimel came to Cedars-Sinai in 2011, and she has held numerous leadership positions including Vice Chair of the Cedars-Sinai Cancer Protocol Review and Monitoring Committee and Associate Director of Gynecologic Oncology Clinical Trials. Her research has focused on clinical trial accrual, recruitment and informed consent.
As the Medical Director for the CCTO, Dr. Rimel will be providing medical guidance and leadership to ensure the quality of services, and she will serve as the CCTO spokesperson for Cedars-Sinai Cancer.
Dr. Rimel is a member of American College of Obstetricians and Gynecologists, Society of Gynecologic Oncologists, American Society of Clinical Oncology, American Association for Cancer Research, and Western Association of Gynecologic Oncologists. Dr. Rimel is a current GOG Foundation/AAOGF Clinician Scientist Awardee for her research entitled, “Olaparib and Durvalumav in Recurrent Progressive Endometrial Cancer: A proposal for a Novel Arm of the Platform Study, NRG GY012.
Congratulations to Dr. Rimel on this outstanding achievement!
AAOGF Scholars Publish in American Journal of Obstetrics & Gyencology
Current scholars Jacqueline G. Parchem, MD and Courtney D. Townsel, MD, MSc along with Sarah A. Wernimont, MD, PhD and Yalda Afshar, MD, PhD have published an article in the American Journal of Obstetrics & Gynecology. The article, “More than grit: growing and sustaining physician-scientists in obstetrics and gynecology,” demonstrates the need for continued support and funding for Women’s Health research.
Click here to read the article.
Clapp Awarded Harvard Risk Management Foundation’s Patient Safety Grant
Dr. Mark Clapp is a maternal-fetal medicine specialist at Massachusetts General Hospital and health services researcher. His research focuses on using big data to improve outcomes during pregnancy and delivery. He recently was awarded the Harvard Risk Management Foundation’s Patient Safety Grant for the project: Leveraging Electronic Health Record Data and Machine-Learning for Neonatal Risk Stratification. This work is a direct extension of the project (Development of an EHR-based Obstetric Risk Score) and training that is supported by the AAOGF/ABOG Research Scholar Award.
The objective of this project is to leverage the power of machine-learning and EHR data within the Mass General Brigham health system to reduce the risk of harm related to fetal distress. Specifically, Dr. Clapp and his team are working to develop and validate a risk prediction tool for adverse neonatal outcomes for use at the start of the second stage of labor. They are also exploring how this tool can be safely and effectively incorporated into clinical practice. The results from this work aim to improve patient safety by increasing provider awareness of risk, improving communication among team members, encouraging patient involvement in their risk prevention strategy, and reducing the impacts of implicit biases introduced in subjective risk assessments. Importantly, this tool is being designed such that it can be easily adapted for other institutions.
Drs. Emily Miller and Jackie Parchem Present at Capitol Hill Briefing
 Drs. Emily Miller and Jackie Parchem, spoke at a virtual Capitol Hill briefing on the need to increase inclusion of pregnant and lactating people in clinical trials using the ongoing COVID-19 pandemic as a case study. (COVID-19 and the Imperative to Include Pregnant and Lactating People in Clinical Trials) Dr. Miller was an AAOGF Bridge Awardee in 2018 for her proposal, “Targeting the Kynureine Pathways in Pregnancy-Related Depression.”
Drs. Emily Miller and Jackie Parchem, spoke at a virtual Capitol Hill briefing on the need to increase inclusion of pregnant and lactating people in clinical trials using the ongoing COVID-19 pandemic as a case study. (COVID-19 and the Imperative to Include Pregnant and Lactating People in Clinical Trials) Dr. Miller was an AAOGF Bridge Awardee in 2018 for her proposal, “Targeting the Kynureine Pathways in Pregnancy-Related Depression.”

Dr. Miller discussed her experiences treating patients during the COVID-19 pandemic, while Dr. Parchem shared her professional and personal insights as a doctor and pregnant person who decided to receive the COVID-19 vaccine. Dr. Parchem is a current SMFM/AAOGF Career Development Awardee for her research entitled, “Modulation of Neural Tube Closure by Amniotic Fluid Exosomes.” Congratulations to Drs. Miller and Parchem on their collective work.
Rajkovic Elected to NAM
Aleksandar Rajkovic, M.D., Ph.D., was elected to the National Academy of Medicine as announced on October 19, 2020. Dr. Rajkovic was an AAOGF-RSDP Scholar from 1999-2002 when he was at Baylor College of Medicine.
Rajkovic is an obstetrician, gynecologist and medical geneticist whose research focuses on basic and translational research in reproductive genomics. His lab investigates the genetic underpinnings of the formation and differentiation of gametes and reproductive tracts and the role of these genes in human disease. For example, they have discovered numerous genes that regulate ovarian follicle formation, the growth of healthy eggs, and genes that cause human infertility.
Another focus is the genetics of fibroid tumors, which are found in nearly a quarter of women by age 45, and therapies to eliminate such tumors. He has been at the forefront of innovative technologies to diagnose and reveal the mechanisms of reproductive pathologies.
Rajkovic joined UCSF in 2018 as the first-ever Chief Genomics Officer of UCSF Health. In this role, he serves as the Medical Director and Chief of the Center for Genetic and Genomic Medicine (CGGM) that organizes, coordinates, and oversees Clinical Genetics and Genomics Services across the entire UCSF Health System. He also serves as the Director of the Genomic Medicine Initiative at UCSF.
Congratulations to Dr. Rajkovic for his outstanding accomplishments!
Secord Awarded Kay Yow Cancer Fund
Angeles Alvarez Secord MD, MHSc, a Professor of Obstetrics and Gynecology at Duke University and Director of Gynecologic Oncology Clinical Trials was recently awarded the Kay Yow Cancer Fund in partnership with the V Foundation for Cancer Research for her project, “Endometrial Cancer Molecularly Targeted Therapy Consortium.” This $1 million award will support the development of a consortium of key stakeholders physicians, scientists, pathologists, and patient advocates committed to defining the use of tumor molecular profiles and biomarkers to direct individualized therapy for women with endometrial cancer.
Dr. Secord is a prior AAOGF/Burroughs Wellcome scholar (2001-2004) and currently the AAOGF Scholar Committee Chair. She recognizes the incredible impact the AAOGF grants in partnership with ABOG, SMFM, and GOG-Foundation have on new and mid-level investigators. During her first year as a Gynecologic Oncology attending she received the AAOGF three-year grant (2001-2004), evaluating the regulation of angiogenesis in ovarian cancer, identifing novel targets and biomarkers to direct anti-angiogentic therapy, and developing clinical trials. Later she received a AAOGF Bridge Grant to evaluate biomarkers that have predictive efficacy for bevacizumab treatment in women with advanced ovarian cancer.
“My career development has surpassed my expectations! The funding and support from AAOGF has been instrumental in my success. I am incredibly excited to be part of a program so committed to the development of academic leaders and researchers in Obstetrics and Gynecology.”
In 2012 the foundation announced an inaugural Bridge Grant Award targeted to support young investigators between mentored research training and successful transition to independently funded investigators.
Scientific Duo Gets Back to Basics to Make Childbirth Safer
Former AAOGF/SMFM scholar Joy-Sarah Y. Vink, MD was recently featured an article published by NPR about her research.
Click here to read the article.
Vink’s lab focuses on understanding how the cervix manages to stay closed in pregnancy and then dramatically remodel to become a soft, compliant structure that is able to dilate and allow for delivery of a fetus.
In addition, her goal is also to understand how this normal process of cervical remodeling goes awry leading to pathologic conditions such as premature cervical failure and spontaneous preterm birth. Currently about one in 10 pregnancies ends prematurely placing these babies at significant risk for complications related to prematurity.
Vink’s goal is to understand how and why the cervix fails prematurely and develop novel therapeutic interventions that will be more effective in keeping the cervix closed to avoid premature births.
“My current success would not be possible without the support and funding from the AAOGF,” she says. “The trajectory of my career in research began with the AAOGF/SMFM Scholarship and I would not be where I am today without the mentorship and support that the AAOGF provided.”
Burd Receives NIH Funding
Irina Burd, MD, PhD is an Associate Professor of Gynecology and Obstetrics and Neurology at the Johns Hopkins University. She was recruited to the Johns Hopkins University to spearhead the development of the field of Fetal Medicine and Fetal Neurology, and is the founder and Director of the Johns Hopkins Integrated Research Center for Fetal Medicine as well as the Director of Maternal Fetal Medicine Fellowship. Prior to coming to the Johns Hopkins University, Dr. Burd earned Bachelor of Arts Degree from Rutgers University (Summa Cum Laude) and completed MD/PhD program at the University of Medicine and Dentistry – Robert Wood Johnson Medical School. She completed her residency in Obstetrics and Gynecology at the Thomas Jefferson University and her fellowship in Maternal Fetal Medicine at the University of Pennsylvania.
During the last year of her MFM fellowship, with the help of ABOG/AAOGF three-year grant (2009-2012), Dr. Burd developed research program studying mechanisms of perinatal brain injury with exposure to intrauterine inflammation. These data allowed Dr. Burd to be successful in her NICHD KO8 application (2012-2017), while at the Johns Hopkins University and under mentorship of a pediatric neurologist. Dr. Burd’s findings on the role of IL1beta in pathogenesis of fetal brain injury with exposure to intrauterine inflammation and infection became very important at the time of Zika infection surge. Receipt of ABOG/AAOGF Bridge grant (2017-2018) allowed her to generate enough preliminary data in her novel Zika model of perinatal brain injury. In 2018, Dr. Burd became a proud recipient of NICHD R01 “IL1beta regulation of perinatal outcomes in Zika infection.”
Dr. Burd has authored more than 100 original papers and scholarly publications, is a member of multiple editorial boards, serves as an Associate Editor for American Journal of Reproductive Immunology and for PloS One as well as an Editor-in-Chief for Obstetrics for a Biomed Central Journal, Maternal Health, Neonatology and Perinatology. Dr. Burd also serves as a Chair of the National Institutes of Health Obstetrics and Maternal Fetal Biology Subcommittee.
AAOGF Scholar Receives K08 Funding
 Jose Alejandro Rauh-Hain is a gynecologic oncologist and a health services researcher at The University of Texas MD Anderson Cancer Center (MDACC). He has extensive experience in analyzing large datasets to evaluate cancer outcomes, including prior work with the linked SEER-Medicare data, SEER, the National Cancer Database, as well as additional experience working with claims data. He has performed comparative effectiveness studies on the surgical management of women with gynecological cancers. In particular, he has authored several publications that have helped to define the role of minimally invasive surgery in gynecologic oncology.
Jose Alejandro Rauh-Hain is a gynecologic oncologist and a health services researcher at The University of Texas MD Anderson Cancer Center (MDACC). He has extensive experience in analyzing large datasets to evaluate cancer outcomes, including prior work with the linked SEER-Medicare data, SEER, the National Cancer Database, as well as additional experience working with claims data. He has performed comparative effectiveness studies on the surgical management of women with gynecological cancers. In particular, he has authored several publications that have helped to define the role of minimally invasive surgery in gynecologic oncology.
These studies demonstrated the oncologic safety of minimally invasive surgery for early stage endometrial cancer, and confirmed that these procedures are safe for staging and interval cytoreductive surgery in women with epithelial ovarian cancer. The latter finding represents the first large study of minimally invasive surgery in advanced ovarian cancer. Contrary to these findings, in a separate paper published in the New England Journal of Medicine, he found that minimally invasive surgery is associated with an elevated risk of death relative to laparotomy in women undergoing radical hysterectomy for early-stage cervical cancer.
He has also a particular interest in examining disparities in gynecological cancer care and studies to improve care of young women with cancer. Specifically, he is interested in descriptive and intervention research studies conducted in real-world clinical settings that have the potential to reveal the effectiveness of strategies for decreasing well-documented disparities in gynecological cancer care access, utilization, and associated clinical outcomes.
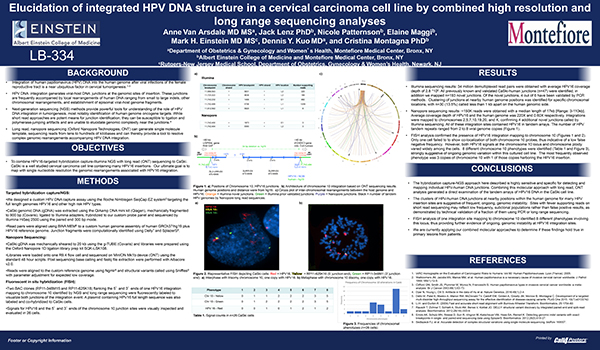
Eludication of Integrated HPV DNA Structure in a Cervical Carcinoma Cell Line by Combined High Resolution and Long Range Sequencing Analyses
Click on the image below to see the work by AAOGF scholar Anne Van Arsdale, MD, MSc.